Revenue cycle management is the backbone of a profitable healthcare practice. Each step from patient registration to final payment impacts cash flow and operational efficiency. This blog will break down the 13 steps of Revenue Cycle Management. These steps will help you optimize everything from patient intake to final collections. We will start from patient registration and move through the whole process step by step.
You’ll understand how front-end processes such as registration and insurance verification lay the groundwork for successful claims and how accurate coding is important. You’ll also gain valuable insights into how reporting and analytics can provide valuable insights for better financial decision-making. This blog is your guide to a streamlined revenue process for increased profitability.
What is Healthcare Revenue Cycle Management?
Healthcare RCM is the financial process used by medical providers to track patient care episodes from initial registration and appointment scheduling to the final payment collection. It is the financial heartbeat of any medical practice. It is the entire system that tracks, manages, and collects money for the services you deliver. Think of it as the bridge connecting clinical care to sustainable operations. Stay connected to explore the 13 steps of revenue cycle management and understand its role in efficient healthcare management.
The 13 Steps of Revenue Cycle Management in Healthcare:
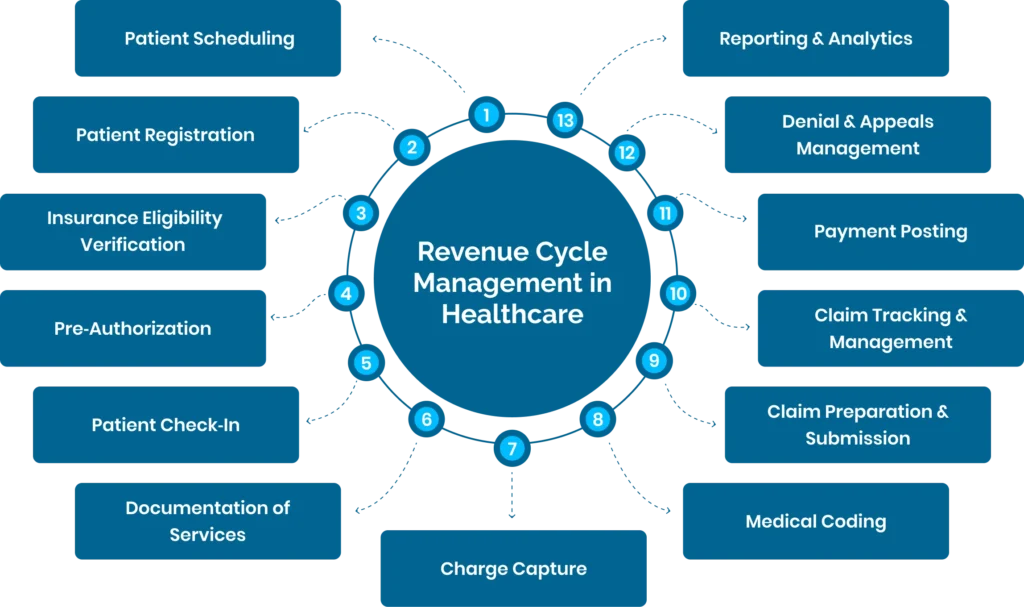
The revenue cycle in healthcare is more than a list of tasks. It is a coordinated flow of actions that turns patient visits into accurate reimbursements and healthy cash flow. Here are the details of all 13 steps of Revenue Cycle Management:
1. Patient Scheduling
This is where the revenue journey begins. It often happens before the patient ever arrives. Smart scheduling ensures accurate contact and insurance data are captured early and appointment slots are used efficiently. The practice can prepare for what the visit will involve. An organized scheduling process reduces no‑shows and builds trust with patients. This step is the first of 13 steps of revenue cycle management.
2. Patient Registration
Demographic details and insurance information are confirmed and documented at registration. Collecting complete and correct data at this stage prevents costly errors later in billing and claims processing. It also gives staff a chance to explain financial policies and what patients can expect on their bills.
3. Insurance Eligibility Verification
Verifying coverage protects both patients and providers. This step confirms the following details of the patient:
- Plan type
- Benefit limits
- Co-pays
- Deductibles
- Any pre‑authorization needs
Claims may be rejected or delayed if eligibility isn’t checked upfront. This leads to lost revenue and frustrated patients. Automation tools can make this step faster and more accurate.
4. Pre‑Authorization
Certain procedures or treatments require insurer approval before they occur. Pre‑authorization ensures the insurer will cover the service. Thus it reduces the risk of denials. Mistakes or delays in this step often lead to claims being denied for “lack of prior approval.” This issue then becomes expensive to resolve.
5. Patient Check‑In
This step reconfirms the patient’s information and collects any upfront payments due upon arrival. Updating records and capturing signatures at check‑in reduces administrative friction later and clarifies the patient’s financial responsibility from the start.
6. Documentation of Services
Every service provided must be documented accurately during the clinical encounter. Detailed documentation includes information related to:
- Diagnoses
- Tests
- Procedures
- Provider notes
These become the foundation for charge capture and coding. Poor documentation can lead to incorrect claims or denials.
7. Charge Capture
Charge capture translates the documented services into billable items. This step ensures all services provided are billed appropriately.
- Record every service delivered during the patient encounter.
- Include tests, procedures, and supplies used.
- Verify that all charges align with insurance requirements.
8. Medical Coding
Medical coding converts clinical documentation into standardized codes (such as ICD‑10, CPT, and HCPCS) that payers use to determine reimbursement. Accuracy is very crucial in this step. Incorrect or missing codes are one of the leading causes of claim denials. Professional coders and regular audits help maintain high coding quality.
9. Claim Preparation and Submission
The claim is assembled and submitted to the insurer once charges are coded. Clean and compliant claims mean they are complete and meet payer rules. They travel through clearinghouses faster and get paid sooner. Errors at this step contribute to delays and rejections.
10. Claim Tracking and Management
Revenue cycle teams actively track claims to ensure they are processed and paid after submission. This may include:
- Following up on pending claims
- Responding to payer requests for additional information
- Quickly correcting issues that arise
Proactive oversight shortens the cash flow timeline.
11. Payment Posting
More of your revenue comes directly from the patient with rising deductibles. This step requires clear communication and empathy.
- Send out easy-to-read and transparent patient statements
- Offer digital payment options for convenience
- Set up manageable payment plans for high-balance accounts
12. Denial and Appeals Management
Some claims are denied even with the best processes in place. This step involves analyzing why a claim was rejected and correcting issues – such as missing documentation or coding errors. And then resubmitting or appealing the claim. Strong denial management recovers revenue that would otherwise be lost.
13. Reporting and Analytics
RCM is not complete without evaluating performance. Revenue leaders review key metrics such as
- Denial rates
- Accounts receivable (A/R) timelines
- Clean claim rates
- Net revenue collected
These insights guide continuous improvement and help to streamline workflows. It also reduces costs and boosts financial outcomes over time.
Healthcare teams can create a more efficient RCM process by being aware of these 13 steps involved in revenue cycle management. This will ensure a robust process that can withstand changing payer requirements and patient demands.
How to Optimize Your 13-Step Revenue Cycle Management Workflow:
Optimization is about working smarter by eliminating the friction points that cause revenue leaks. Manual data entry and chasing payers are the biggest drains on your resources in the 2026 healthcare climate. To refine your 13 steps of revenue cycle management process, it is essential to concentrate on these three key areas:
- Automation: There should be automation of repetitive processes such as eligibility and claims scrubbing. Your staff will have no time to concentrate on intricate issues if they are manually engaged in repetitive processes. Transformative technology like AI automation should handle these tasks.
- Prioritize Front-End Accuracy: Most denials are born at the registration desk. You ensure that the information entering the cycle is 100% accurate before any clinical work begins by implementing “real-time” verification tools.
- Leverage Specialized Expertise: The best way to optimize is to know when to bring in the pros. This is where a partner like Paymedics becomes invaluable. They specialize in transforming these 13 steps from a disjointed administrative burden into a streamlined process. You gain access to advanced analytics and certified coders by integrating professional RCM services.
Ready to streamline your revenue cycle and reduce costly billing errors? Partner with Paymedics today to optimize your 13 steps of Revenue Cycle Management workflow.
Frequently Asked Questions
How many steps are there in RCM?
There are 13 steps of revenue cycle management. These steps are fundamental and beneficial for healthcare organizations. It ensures they are generating enough revenue to maintain their operations.
What are the three main pillars of revenue cycle management?
The three pillars of healthcare RCM are:
- People
- Process
- Technology
A balanced integration of these elemetns is essential for optimizing financial health and managing the entire patient encounter lifecycle from scheduling to final payment.
Should I automate the 13 steps of reveneue cycle management?
Automating the 13 steps of RCM is very beneficial for your healthcare organization. Automation handles boring tasks so you can focus on more complex cases. It also reduces manual erros and accelerates cash flow.
Why does RCM matter so much for small practices?
Csah flow is everything when you have a small practice or specialty-focused clinic. All your operations can be impacted if claims are denied or payments drag on. Good RCM means predictable revenue and more focus on patients.
Is it better to keep RCM in-house or outsource it?
It depends on your size. Small practices have a hard time keeping up with changing regulations. That’s why it’s a lot cheaper to work with a company such as Paymedics.
Why are the 13 steps of Revenue Cycle Management important?
Each step plays a role in ensuring healthcare providers are paid correctly and on time. These steps create a more stable cash flow for healthcare organizations when they are followed carefully.
What are the four Ps of RCM?
The four Ps of revenue cycle management in healthcare are:
- Patient: Accurate info, clear expectations, smooth engagement upfront
- Provider: Proper documentation, accurate coding, full compliance
- Payer: Coverage verification, clean claims, efficient adjudication
- Process: Streamlined workflows, error reduction, continuous optimization
Which step is important out of the 13 steps of revenue cycle management?
All 13 steps of Revenue Cycle Management are interconnected. But Patient Pre-registration/Registration and Insurance Eligibility Verification are generally considered the most critical steps.





